Tests
A number of different tests can be performed to assess people
with achalasia, to look for other common causes of the same
symptoms and make a definite diagnosis.
Upper GI endoscopy
The first test to investigate difficulty in swallowing is
usually an upper GI endoscopy (often referred to as an OGD). This
is a common procedure involving the insertion of a thin tube with a
camera on the end through the mouth into the oesophagus, stomach
and first part of the small bowel called the duodenum. This test is
important to look for signs of achalasia as well as to look for
other problems such as acid damage or oesophageal cancer. It is a
very routine procedure, but as with any test there are benefits and
risks, even though the risks are very low. More information on this
procedure, its benefits and risks are available
here.
Contrast swallow
This test may also be called a barium swallow and is often
combined with a meal test to examine the stomach as well as the
oesophagus. It involves drinking some fluid (called barium) and
having x-ray pictures taken of the fluid going down the oesophagus
into the stomach. This is a good test of how the oesophagus
squeezes and is very helpful in making a diagnosis of achalasia
(see figure 1).
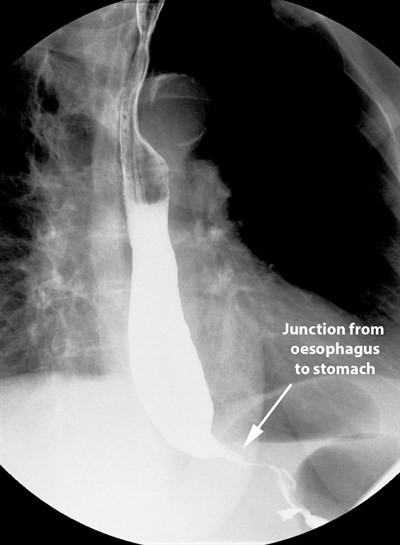
Figure 1. Appearance of achalasia on barium swallow. Source:
UHBW NHS Foundation Trust, 2021.
pH and manometry
These two tests (pH testing and manometry) are often combined to
assess a range of symptoms. They involve passing a fine tube
through the nose into the oesophagus, then doing a series of
swallowing tests to measure how the oesophagus works (the manometry
part of the test). A tube is then left in place for 24 hours and
you go home with this before having it removed the following day
(pH testing). During this period, you can record symptoms that you
experience which can then be looked at together with measurements
from the tube.